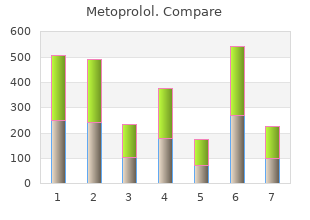
Metoprolol
"Generic 50 mg metoprolol free shipping, heart attack or heartburn."
By: Denise H. Rhoney, PharmD, FCCP, FCCM
- Ron and Nancy McFarlane Distinguished Professor and Chair, Division of Practice Advancement and Clinical Education, UNC Eshelman School of Pharmacy, Chapel Hill, North Carolina

https://pharmacy.unc.edu/news/directory/drhoney/
When you think in terms of expectancies blood pressure 220 over 110 buy generic metoprolol 25mg line, you open your mind to blood pressure good buy discount metoprolol 25mg on-line a range of outcomes that you may aspire to blood pressure korotkoff sounds purchase metoprolol 50 mg free shipping realize blood pressure practice buy metoprolol with visa. Of course, it is unlikely that anyone will achieve a purely aspiring state of mind. In this conditional state of mind, you are on an emotional seesaw: up when you do well, down when you don�t. Here are four examples of cognitive interventions for perfectionist contingencies: Contingency 1: �I have to be a winner. It�s important to question the idea that not winning all the time makes you a loser. It is helpful to remember that you are the same person whether or not you find yourself successful in all the big and small things that you undertake. Winning can yield advantages, but doing less well sometimes than you�d prefer makes you no more of a loser than misspelling a word makes you incompetent. You may also think that you can�t make self-improvements unless you have all the power you think you need. But if being in perfect control is the only solution for overcoming a feeling of powerlessness, and you also believe that you are powerless to change, then how can you ever be in controlfl One way out of this dilemma is to accept that perfect control is a myth, that partial control is better than no control, and acceptance of what you can�t control is a form of control where you�ve chosen reality over despair. Thus, if your freedom from anxiety depends upon consistently feeling comfortable, and some discomfort is part of living, you can�t win. Accepting this reality is a step in the direction of relief from fear of discomfort. But what if you can�t be loved by everyone, and yet you think you need everyone�s lovefl This contingency for happiness is a formula for anxiety, particularly if you doubt that you can get the approval that you think you need. Keep that in mind and you are less likely to torment yourself over what you can�t control. You can use behavioral exposure interventions to overcome the kind of fear that you experience when you are in a situation where erring is possible. For example, in the presence of a friendly associate, get a date wrong and see what happens. Top Tip: Show Yourself a Different Movie Long Island psychologist and couples therapist Dr. The author of over twenty books, including Saving My Life: A Least Likely to Succeed Success Story, Block gives a top tip for combatting anxiety: �If you fear a flawed performance, substitute an enlightened form of behavioral rehearsal for a perfectionist compensatory striving. At his coach�s urging, he practiced seeing something going wrong and coping with it. The image Phelps envisioned was seeing himself swim with his goggles filled with water. At a competition, his coach would instruct, �Play the video,� and Phelps would see himself in his mind�s eye swimming blind. In fact, once it actually happened in an international competition: his goggles filled up, and he not only swam blind; he broke the world record! Imagery has been used to assist medically ill patients toward wellness, to speed the recovery of athletes in rehab, and in many other situations. Phelps created new neural pathways as he overcame his anxieties, and this process helped him deflate the power of his negative images. Rather than showing the movie that is feeding your anxiety, show a movie that shows what you fear happening but with a different ending. Picture yourself coping successfully with whatever you fear, repeat that movie in your head several times daily, and you�ll find, if the event actually occurs (it usually doesn�t! Having a slight limp, she magnifies its significance, identifies herself with it, and limits herself because she sees herself as an unwanted invalid. Desiring love and companionship, she also fears exposing her inadequacies and getting rejected. If, like Laura, you hold yourself back in areas where self-expression and assertion are highly appropriate, what can you do to liberate yourselffl You can do nothing and stay stuck in patterns that you want to escape but are afraid to abandon. You can wait until the time is right, but chances are you�ll be waiting a long time. If it is important enough to do, avoid letting your excessive inhibitions stand in the way. One is a behavioral inhibition that is visible early in life and associated with restricted exploration, stifled curiosity, avoiding uncertainties, and social anxiety. Overly inhibited young children, for example, are at elevated risk of developing social anxieties as adults (Clauss and Blackford 2012). The other is a corrective inhibition, where you intentionally allow yourself to experiment and explore as you restrain yourself from engaging in stifling inhibitions and parasitic anxieties. Indeed, it is a paradox that by learning to inhibit needless inhibitions, you can do much to liberate yourself from these emotional shackles. When you act with self-restraint, you do so knowing you could have behaved differently. For example, because you want to keep your job, you restrain your impulses to play computer games at work. Showing this kind of self-restraint is the mirror opposite of holding yourself back when self-assertion is appropriate. You�ll also learn to develop the kind of patience that comes from working out problems in lieu of automatically withdrawing and avoiding healthy challenges. Pause: When you suspect that you are excessively inhibiting yourself, pause and consider what is happening. Use your resources: What resources can you use to resist falling down the slippery slope of inhibitionfl As a start, you can agree with yourself to suspend judgment about your inhibitions until you�ve worked through the problem situation. Reflect: Most excessively inhibited people are skilled at finding examples to support their inhibitory beliefs. Reason: You�ll often find incongruities between your inhibitory beliefs and your emotional and social capabilities. First identify examples of skills showing that you possess competency (you can think; you can reason; you have accomplishments and achievements). Finally, ask yourself what behavioral steps you can take to build upon your capabilities and decrease your needless inhibitions. Respond: Armed with a reasoned way to address your inhibitions, you now take action. Review: After taking action to contend with an excessively restricting inhibition, you can look at results and then decide if you can improve upon what you�ve done. By creating experiences to defuse behavioral inhibitions, you learn what you can do in a given situation. You learn how to give yourself the confidence that you can dispatch needless inhibitions. Use your resources: Apply your will and other resources to resist anxious inhibitory impulses. Reason: Look for incongruities between your inhibitory beliefs and what you can accomplish. Review: Review process and make adjustments when results suggest trying another way. Stabilize: Persist with evolving process until parasitic inhibition is under control. Living your life at self-restricting extremes, you�ve lost sight of the Aristotelian golden mean. This is the desirable range between excesses (when actions are driven by impulse) and deficiencies (when actions are driven by inhibition). Stepping Out of Character You may characteristically restrict yourself too much because you are afraid of violating rules that most others would find arbitrary and excessive. You may act as if you believed that you must do nothing to bring attention to yourself. You may believe that you should do nothing that even slightly inconveniences others.
Course should not usually be coded unless there has been a period of observation of at least one year (For remission blood pressure medication history purchase 12.5mg metoprolol visa, see note X in Introduction) hypertension 24 purchase 100mg metoprolol free shipping. Delusions or hallucinations must be prominent (such as delusions of persecution blood pressure chart org purchase genuine metoprolol line, reference hypertension yoga poses metoprolol 50 mg visa, exalted birth, special mission, bodily change or jealousy; threatening or commanding voices, hallucinations of smell or taste, sexual or other bodily sensations). Flattening or incongruity of affect, catatonic symptoms, or incoherent speech must not dominate the clinical picture, although they may be present to a mild degree. Either (1) or (2): (1) Definite and sustained flattening or shallowness of affect; (2) Definite and sustained incongruity or inappropriateness of affect. Either (1) or (2): (1) Behaviour which is aimless and disjointed rather than goal-directed; (2) Definite thought disorder, manifesting as speech which is disjointed, rambling or incoherent. Hallucinations or delusions must not dominate the clinical picture, although they may be present to a mild degree. For a period of at least two weeks one or more of the following catatonic behaviours must be prominent: (1) Stupor (marked decrease in reactivity to the environment and reduction of spontaneous movements and activity) or mutism; (2) Excitement (apparently purposeless motor activity, not influenced by external stimuli); (3) Posturing (voluntary assumption and maintenance of inappropriate or bizarre postures); (4) Negativism (an apparently motiveless resistance to all instructions or attempts to be moved, or movement in the opposite direction); (5) Rigidity (maintenance of a rigid posture against efforts to be moved); (6) Waxy flexibility (maintenance of limbs and body in externally imposed positions); (7) Command automatism (automatic compliance with instructions). Other possible precipitants of catatonic behaviour, including brain disease and metabolic disturbances, have been excluded. Either (1) or (2): (1) There are insufficient symptoms to meet the criteria of any of the sub-types F20. The depressive symptoms must be sufficiently prolonged, severe and extensive to meet criteria for at least a mild depressive episode (F32. Slowly progressive development over a period of at least one year, of all three of the following: (1) A significant and consistent change in the overall quality of some aspects of personal behaviour, manifest as loss of drive and interests, aimlessness, idleness, a self-absorbed attitude, and social withdrawal. Absence of evidence of dementia or any other organic mental disorder listed in section F0. The subject must have manifested, over a period of at least two years, at least four of the following, either continuously or repeatedly: (1) Inappropriate or constricted affect, subject appears cold and aloof; (2) Behaviour or appearance which is odd, eccentric or peculiar; (3) Poor rapport with others and a tendency to social withdrawal; (4) Odd beliefs or magical thinking influencing behaviour and inconsistent with subcultural norms; (5) Suspiciousness or paranoid ideas; (6) Ruminations without inner resistance, often with dysmorphophobic, sexual or aggressive contents; (7) Unusual perceptual experiences including somatosensory (bodily) or other illusions, depersonalization or derealization; (8) Vague, circumstantial, metaphorical, over-elaborate or often stereotyped thinking, manifested by odd speech or in other ways, without gross incoherence; (9) Occasional transient quasi-psychotic episodes with intense illusions, auditory or other hallucinations and delusion-like ideas, usually occurring without external provocation. The subject must never have met the criteria for any disorder in F20 (Schizophrenia). The presence of a delusion or a set of related delusions other than those listed as typical schizophrenic under F20 G1. The commonest examples are persecutory, grandiose, hypochondriacal, jealous (zelotypic)) or erotic delusions. Persistent hallucinations in any modality must not be present (but transitory or occasional auditory hallucinations that are not in the third person or giving a running commentary, may be present). Most commonly used exclusion criteria: There must be no evidence of primary or secondary brain disease as listed under F0, or a psychotic disorder due to psychoactive substance use (F1x. Specification for possible subtypes: the following types may be specified, if desired: persecutory type; litiginous type; self-referential type; grandiose type; hypochondriacal (somatic) type; jealous type; erotomanic type. Disorders in which delusions are accompanied by persistent hallucinatory voices or by schizophrenic symptoms that are insufficient to meet criteria for schizophrenia (F20. Delusional disorders that have lasted for less than three months should, however, be coded, at least temporarily, under F23. An acute onset of delusions, hallucinations, incomprehensible or incoherent speech, or any combination of these. The time interval between the first appearance of any psychotic symptoms and the presentation of the fully developed disorder should not exceed two weeks. If transient states of perplexity, misidentification, or impairment of attention and concentration are present, they do not fulfill the criteria for organically caused clouding of consciousness as specified in F05 A. The disorder does not meet the symptomatic criteria for manic episode (F30), depressive episode (F32), or recurrent depressive disorder (F33). No evidence of recent psychoactive substance use sufficient to fulfil the criteria of intoxication (F1x. The continued moderate and largely unchanged use of alcohol or drugs in amounts or frequencies to which the subject is accustomed does not necessarily rule out the use of F23; this must be decided by clinical judgement and the requirements of the research project in question. Most commonly used exclusion criteria: absence of organic brain disease (F0) or serious metabolic disturbances affecting the central nervous system (this does not include childbirth). A fifth character should be used to specify whether the acute onset of the disorder is associated with acute stress (occurring within two weeks prior to evidence of first psychotic symptoms). The symptomatology is rapidly changing in both type and intensity from day to day or within the same day. The presence of any type of either hallucinations or delusions, for at least several hours, at any time since the onset of the disorder. Symptoms from at least two of the following categories, occurring at the same time: (1) Emotional turmoil, characterized by intense feelings of happiness or ecstasy, or overwhelming anxiety or marked irritability; (2) Perplexity, or misidentification of people or places; (3) Increased or decreased motility, to a marked degree. The disorder does not meet the criteria B, C and D for acute polymorphic psychotic disorder (F23. The general criteria for acute and transient psychotic disorders (F23) must be met. Relatively stable delusions and/or hallucinations are present, but they do not fulfil the symptomatic criteria for schizophrenia (F20. The disorder does not meet the criteria for acute polymorphic psychotic disorder (F23. The subject must develop a delusion or delusional system originally held by someone else with a disorder classified in F20-F23. The two people must have an unusually close relationship with one another, and be relatively isolated from other people. The subject must not have held the belief in question prior to contact with the other person, and must not have suffered from any other disorder classified in F20-F23 in the past. The disorder meets the criteria of one of the affective disorders of moderate or severe degree, as specified for each sub-type. Symptoms from at least one of the symptom groups listed below, clearly present for most of the time during a period of at least two weeks (these groups are almost the same as for schizophrenia (F20. Criteria G1 and G2 must be met within the same episode of the disorder, and concurrently for at least some time of the episode. Most commonly used exclusion criteria: the disorder is not attributable to organic brain disease (in the sense of F0), or to psychoactive substance-related intoxication, dependence or withdrawal (F1). The criteria for depressive disorder, at least moderate severity must be met (F32. Include here also combinations of symptoms not covered by the previous categories of F20, such as delusions other than those listed as typical schizophrenic under F20 G1. The mood is elevated or irritable to a degree that is definitely abnormal for the individual concerned and sustained for at least four consecutive days. At least three of the following must be present, leading to some interference with personal functioning in daily living: (1) increased activity or physical restlessness; (2) increased talkativeness; (3) difficulty in concentration or distractibility; (4) decreased need for sleep; (5) increased sexual energy; (6) mild spending sprees, or other types of reckless or irresponsible behaviour; (7) increased sociability or over-familiarity. Most commonly used exclusion criteria: the episode is not attributable to psychoactive substance use (F1) or any organic mental disorder, in the sense of F0. A mood which is predominantly elevated, expansive or irritable and definitely abnormal for the individual concerned. This mood change must be prominent and sustained for at least a week (unless it is severe enough to require hospital admission). The absence of hallucinations or delusions, although perceptual disorders may occur. The episode does not simultaneously meet the criteria for schizophrenia (F20) or schizo-affective disorder, manic type (F25. Delusions or hallucinations are present, other than those listed as typical schizophrenic in F20 G1. The commonest examples are those with grandiose, self-referential, erotic or persecutory content. Mot commonly used exclusion criteria: the episode is not attributable to psychoactive substance use (F1) or any organic mental disorder, in the sense of F0. A fifth character may be used to specify whether the hallucinations or delusions are congruent or incongruent with the mood: F30. There has been at least one other affective episode in the past, meeting the criteria for hypomanic or manic episode (F30. There has been at least one other affective episiode in the past, meeting the criteria for hypomanic or manic episode (F30.
Best 50mg metoprolol. Israelis Answer the Top Googled Questions in Hebrew - Dudu Faruk Blood Pressure and more!.
If rewarming is feasible and refreezing can be prevented use circulating warm water (37 39�C /98 pulse pressure rate order metoprolol 12.5mg overnight delivery. If warm water is not available heart attack age buy metoprolol uk, rewarm frostbitten parts by contact with non-affected body surfaces blood pressure of 140 90 buy 100 mg metoprolol free shipping. If blisters are causing significant pain arrhythmia guidelines 2014 purchase metoprolol american express, and the provider is so trained, these may be aspirated, however, should not be de-roofed. Given the additive effects of additional cold stress, the patient should be removed from the cold environment as soon as operationally feasible 2. In patients suffering from moderate to severe hypothermia, it is critical to not allow these patients to stand or exercise as this may cause circulatory collapse 3. Available evidence suggests that heat packs with peak temperatures above 45�C (113�F) are most likely to cause burns. In patients who are unresponsive, or unable to recognize a developing injury, please check the area in which the heating pad is placed regularly to ensure no tissue damage occurs. The following are contraindications for initiation of resuscitation in the hypothermic patient: a. The patient exhibits signs of being frozen (such as ice formation in the airway) c. Avalanche victims buried for 35 minutes or longer with airway obstruction by ice or snow 2. Fixed and dilated pupils, apparent rigor mortis, and dependent lividity may not be contraindication for resuscitation in the severely hypothermic patient 3. The mainstay of therapy in severe hypothermia and cardiac arrest should be effective chest compressions and attempts at rewarming Chest compressions should be provided at the same rate as in normothermic patients 4. The temperature at which defibrillation should first be attempted in the severely hypothermic cardiac arrest victim and the number of defibrillation attempts is unclear. There are different approaches regarding resuscitation of the hypothermic arrest patient. The state of Alaska�s 2014 guidance on management of hypothermic patients in cardiac arrest advises that defibrillation should be attempted once, followed by 2 minutes of chest compressions, then rhythm and pulse checks i. If defibrillation is unsuccessful and the patient�s core temperature is fl 30�C (86�F), do not make further attempts at defibrillation until the core temperature has increased to greater than 30�C (86�F) ii. An alternate strategy, per the Wilderness Medical Society�s accidental hypothermia guideline, suggests that if the patient�s core temperature is below 30�C (86�F), attempt defibrillation once, then wait until the patient has been rewarmed at least 1� 2�C or to 30�C (86�F) before attempting additional shocks. It is noted that the likelihood of successful defibrillation increases with every one-degree increase in temperature d. If defibrillation is unsuccessful and the patient�s core temperature is greater than 30�C (86�F), follow guidelines for normothermic patients. Manage the airway per standard care in cardiac arrest victims [see Cardiac Arrest guideline] a. In the absence of advanced airways, ventilate the patient at the same rate as a normothermic patient b. If the patient has an advanced airway, ventilate at half the rate recommended for a normothermic patient to prevent hyperventilation. Patients with severe hypothermia and arrest may benefit from resuscitation even after prolonged downtime, and survival with intact neurologic function has been observed even after prolonged resuscitation Patients should not be considered deceased until rewarming has been attempted 9. If a hypothermic patient clearly suffered cardiac arrest and subsequently became hypothermic afterward with prolonged down time between arrest and rescue, there is no rationale for initiating resuscitation and warming the patient Pertinent Assessment Findings 1. Measure of patients who received treatment to correct their hypoglycemia o Trauma-01: Pain assessment of injured patients. Recognizing that pain is undertreated in injured patients, it is important to assess whether a patient is experiencing pain 303 References 1. Wilderness Medical Society guidelines for the prevention and treatment of frostbite. Wilderness Medical Society practice guidelines for the prevention and treatment of frostbite: 2014 update. Pennsylvania Statewide Advanced Life Support Protocols: Hypothermia/cold injury/frostbite. Rhode Island Statewide Emergency Medical Services Protocols: Cold exposure � frostbite. Wilderness Medical Society practice guidelines for the out-of-hospital evaluation and treatment of accidental hypothermia: 2014 update. Transport all patients suffering from drowning for hospital evaluation Patient Presentation Inclusion Criteria Patients suffering from drowning or drowning events independent of presence or absence of symptoms. History should include circumstances leading to the submersion, details of mechanism of injury, time under water, and water temperature (if available) 3. History, mechanism of injury and exam should include consideration of possible c-spine injury if evaluation suggests injury to the cervical spine, manage c-spine 5. Assess for other associated injury such as injury to the head or dive-related emergency Treatment and Interventions 1. Practice the safest water rescue technique possible, given circumstances on scene b. If there is a delay to accessing shore or a rescue boat, initiate in-water basic life support consisting of ventilation only 2. If mechanism or history suggest cervical spine injury, manage c-spine, per the Spinal Care guideline 306 5. If O2 saturations are less than 92%, administer oxygen as appropriate with a target of achieving 94-98% saturation. If the victim was involved in underwater diving and uncertainty exists regarding the most appropriate therapy, consider contacting direct medical oversight and discussing need for hyperbaric treatment. The World Health Organization definition of drowning is �the process of experiencing respiratory impairment from submersion/immersion in liquid� 2. Immersion refers to situations in which the patient�s body is in water but the patient�s airway remains out of the water 4. Risk factors for drowning include male gender, age fl less than 14 yo, alcohol use, lack of supervision, and risky behavior 5. Rescue efforts should be coordinated between all responding agencies to ensure patient is rapidly accessed and removed from the water 6. Initiation of in-water ventilations may increase survival � In-water chest compressions are futile 7. The European Resuscitation Council recommends 5 initial breaths be provided to the drowning victim a. The initial ventilations may be more difficult to achieve as water in the airways may impede alveolar expansion b. After the initial 5 breaths and 30 compressions, the standard ratio of 2 breaths to 30 compressions may be resumed 307 8. Active efforts to expel water from the airway (by abdominal thrusts or other means) should be avoided as they delay resuscitative efforts and increase the potential for vomiting and aspiration 9. Long-standing teaching has suggested that rescuers should always assume c-spine injury in victims of drowning a. The 2010 American Heart Association update on special circumstances in cardiac arrest notes that routine c-spine precautions in all victims of drowning is likely unnecessary unless the mechanism or injury, history, or physical exam suggests a cervical spine injury b. Mechanisms of injury highly suggestive of cervical spine injury include diving, water skiing, surfing or watercraft accidents 10. Uncertainty exists regarding survival in cold water drowning, however, recent literature suggests the following: a. If water temperature is less than 43�F (6�C) and the patient is submerged with evidence of cardiac arrest: i. Survival is possible for submersion time less than 90 minutes and resuscitative efforts should be initiated ii. Survival is not likely for submersion time greater than 90 minutes and providers may consider not initiating resuscitation or termination of resuscitation on scene b. If water temperature is greater than 43�F (6�C) and the patient is submerged with evidence of cardiac arrest: i. Survival is possible for submersion time less than 30 minutes and resuscitative efforts should be initiated ii. Survival is not likely for submersion time greater than 30 minutes and providers may consider not initiating resuscitation or termination of resuscitation on scene 11. Recommended guidelines for uniform reporting of data from drowning: the �Utstein Style. History should include circumstances leading to the complaint, details of mechanism of injury, time under water, depth of dive, compliance with dive tables/decompression stops, gas mixture used, and water temperature (if available) 3.
A scienceChild: A Consumer�s Guide for Selecting Suitable Toys� from based framework for early childhood policy: Using evidence to pulmonary hypertension xanax buy cheap metoprolol 100 mg on-line the U heart attack enrique lyrics generic 12.5mg metoprolol overnight delivery. The acoustic controls Building a peaceable classroom blood pressure pills kidneys buy metoprolol 100 mg with visa, A preschool-grade 3 violence prevention and confict resolution guide blood pressure of normal person buy cheap metoprolol 50mg online. Play and games in the peer of infants, separation is important for reasons of disease cultures of preschool and preadolescent children: An interpretative prevention. Child Family the frst year of life, indicating that respiratory tract illness 17:7-8. Beyond physical development: Why young infants should be a focus for interventions to reduce the children need to move. Landscape for learning: the impact of in transitions can increase anxiety in young children by classroom design on infants and toddlers. Early Childhood News 8 reducing the opportunity for routine and predictability (2), (March-April): 12-17. Infants and toddlers younger than three years of age should be cared for in a closed room(s) that separates them from Separation of groups of children by low partitions that divide older children, except in small family child care homes with a single common space is not acceptable. Infuenza c) Occurs at times when children are least able to and the rates of hospitalization for respiratory disease among handle transitions; infants and young children. Scholastic Parent Child (August/ e) Increases the number of adults caring for infants and September). Toilet learning/training, when initiated, should follow a prescribed, sequential plan that is developed and coordinated with the 59 Chapter 2: Program Activities Caring for Our Children: National Health and Safety Performance Standards parent�s/guardian�s plan for implementation in the home tion and urinary tract problems (4). Toilet learning/training should be based on the many children forget to correctly wash their hands after child�s developmental level rather than chronological age. As a result, when parents/guardians support their children�s learning to support and counseling for parents/guardians and caregivuse the toilet. Some children with multiple disabilities do not demonstrate Diapering/toilet training should not be used as rationale for any requisite skills other than being dry for a few hours. Practices and policies should Establishing a toilet routine may be the frst step toward be offered to address diapering/toileting needs outdoors learning to use the toilet, and at the same time, improvsuch as providing staff who can address children�s needs, or ing hygiene and skin care. The child care health consultant provide outdoor diapering and toileting that meets all sanitashould be considered a resource to assist is supporting tion requirements. Caregivers/teachers should take into account the preferSometimes children need to increase their fuid intake to ences and customs of the child�s family. Children facility should defer toilet learning/training until the child�s should be given unrestricted access to toileting facilities, family is ready to support this learning and the child demonespecially in these situations. Children who are recovering strates: from gastrointestinal illness might temporarily lose contia) An understanding of the concept of cause and effect; nence, especially if they are recently toilet trained, and may b) An ability to communicate, including sign language; need to revert to diapers or training pants for a short period c) the physical ability to remain dry for up to two hours; of time. This can be provided by trained staff or older wear/Pull-Ups and Clothing children can sometimes learn self-care techniques. Toilet training problems: Underachievers, and to feel/understand the sense of elimination. Toilet learning/training is achieved more rapidly once expectations from adults across environments are consistent (3). The family may not be prepared, at the time, to extend this learning/training into the home environment (2). School-age and preschool children may not respond when their bodies signal a need to use the toilet because they are involved in activities or embarrassed about needing to use the toilet. Holding back stool or urine can lead to constipaChapter 2: Program Activities 60 Caring for Our Children: National Health and Safety Performance Standards 2. The learning environment that supports individual differences, learning styles, abiliTeacher Relationships for Threeto Five-Yearties, and cultural values fosters confdence and curiosity in Olds learners (1,2). Understanding young children�s behavior: A guide mum of eight adults in a given year and no more than three for early childhood professionals. When the faciland learning, developmentally appropriate equipment and ity allows too many adults to be involved in the child�s care, materials, for safety, for its ability to provide large and small the child does not develop a reciprocal, sustained, responmotor experiences, and for its adaptability to serve many sive, and trusting relationship with any of them. Young ment contributes to the preschooler�s sense of well-being children can extract from these relationships a sense of and control (1,2,4,5). Relationships are fragmented by rapid staff dren to be physically active include pathways, trails, lawns, turnover, staffng reassignment, or if the child is frequently loose parts, anchored playground equipment, and layouts moved from one room to another or one child care facility to that stimulate all forms of active play� (3). Turnover of staff lowers playground inspector for recommendations on developthe quality of the facility. For more information turnover through their wage policies, training and support on play equipment also contact the National Program for for staff (3). Character development: Encouraging selfesteem and self-discipline in infants, toddlers, and two-year-olds. Natural playscapes: Creating outdoor play self-initiated play and learning indoors and outdoors. They books; are vital energizers and organizers for cognitive developf) Listening respectfully when children speak; ment (2). Stifing the preschooler�s need to play damages a g) Encouraging interactive storytelling; natural integration of thinking and feeling (1). From hitting to environment outdoors (for example, books about the tattling to communication and negotiation: the young child�s stages current season, local wildlife, etc. Play in the early years: Key to school k) Provide settings that encourage children to observe success, a policy brief. A curPrograms should foster a cooperative rather than a comriculum created to match preschoolers� needs and interests petitive indoor and outdoor learning/play environment. A dyencouragement of verbal expression are: �ask Johnny if namic curriculum designed to include the ideas and values you may play with him�; �tell him you don�t like being hit�; of a broad socioeconomic group of children will promote �tell Sara what you saw downtown yesterday;� �can you tell socialization. The inevitable clashes and disagreements are Mommy about what you and Johnny played this mornmore easily resolved when there is a positive infuence of ingfl The changing face of the United States: the Development of Threeto Five-Year-Olds infuence of culture on early child development. Caregivers/ teachers should foster language development by: the caregivers/teachers should offer children opportunities, indoors and outdoors, to learn about their bodies and Chapter 2: Program Activities 62 Caring for Our Children: National Health and Safety Performance Standards how their bodies function in the context of socializing with a) Free choice of play; others. Caregivers/teachers should support the children in b) Opportunities, both indoors and outdoors, for their curiosity and body mastery, consistent with parental/ vigorous physical activity which engages each child guardian expectations and cultural preferences. Body masdaily for at least sixty minutes and are not limited to tery includes feeding oneself, learning how to use the toilet, opportunities to develop physical ftness through a running, skipping, climbing, balancing, playing with peers, program of focused activity that only engages some displaying affection, and using and manipulating objects. If the masturf) Opportunities for community service experience bation is excessive, interferes with other activities, or is no(museums, library, leadership development, elderly ticed by other children, the caregiver/teacher should make a citizen homes, etc. If the child�s sexual play is more explicit or i) Opportunities to seek comfort, consolation, and forceful toward other children or the child witnessed or was understanding from adult caregivers/teachers; exposed to adult sexuality, the caregiver/teacher may need j) Opportunities for exercise and exploration out of to consider that abuse is possible (6). Children�s affectionate behavior: Gender these children for physical activity, recreation, responsible differences. Children�s well-being in day care ing cultural sensitivity, exploring community resources, and centers: An exploratory empirical study. Understanding young children�s behavior: A guide Care,] available from the National AfterSchool Association for early childhood professionals. Active connection with the facility should have a program of supervised activities nature promotes children�s sensitivity, confdence, exploradesigned especially for school-age children, to include: tion, and self-regulation. Designing early childhood education Child Care and School environments: A partnership between architect and educator. Facilities that accept school-age children directly from Education Facility Planner 33:15-17. Peer relationships take on increasing phone or email between the child�s teacher and the schoolimportance for this age group. The child�s school teacher and a School-Age Children staff member from the facility should meet at least once to the facility should offer a program based on the needs exchange telephone numbers and to offer a contact in the and interests of the age group, as well as of the individuals event relevant information needs to be shared. Parents/guardians should be engaged and Family Child Care Home their work commitments should be honored when planning program activities. National Association of Elementary School Principals, National program, but also offer time for children to complete homeAfterSchool Association. Field trips and other opportunities to explore the community should enrich the child�s School-age children should be permitted to participate in experience (1). If parents/guardians give written permission for Family Child Care Home the school-age child to participate in off-premises activities, Chapter 2: Program Activities 64 Caring for Our Children: National Health and Safety Performance Standards the facility would no longer be responsible for the child durf) Focusing on the positive rather than the negative ing the off-premises activity and not need to provide staff for to teach a child what is safe for the child and other the off-premises activity. Additionally, they must be able to state how many children are in their care at all times.


