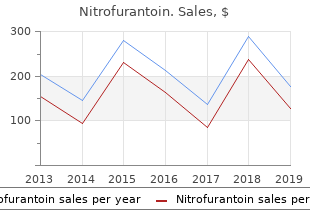
Nitrofurantoin
"Purchase nitrofurantoin without a prescription, antibiotic yeast infection male."
By: Denise H. Rhoney, PharmD, FCCP, FCCM
- Ron and Nancy McFarlane Distinguished Professor and Chair, Division of Practice Advancement and Clinical Education, UNC Eshelman School of Pharmacy, Chapel Hill, North Carolina

https://pharmacy.unc.edu/news/directory/drhoney/
Elizabeth and Betty shared life stories before Elizabeth admitted she was a spy and allowed Betty to antimicrobial effects of spices order nitrofurantoin 50 mg overnight delivery die by overdosing on heart medicine antibiotic resistance action center order nitrofurantoin discount. This was said with his dying breath antibiotic 3 pack purchase 50mg nitrofurantoin free shipping, ending that storyline but opening the door for a major new one antibiotics insomnia discount nitrofurantoin 50mg without prescription. The sixth and final season was splendid and "The Summit," which was the eighth of ten episodes, was great. It featured Philip revealing to Elizabeth that he had been reporting on her activities. Although she was upset at first, you could see that Elizabeth was starting to realize that Philip was right. Whatever else happened in the episode almost seems irrelevant, even if it was good. That sabotaged their overarching mission and added another wrinkle to his rift with Elizabeth. Paige called her mother a whore and left after Elizabeth scolded her on the differences in their lives. They had the showdown fans waited for since the premiere episode, as Stan finally caught them. EmbA and EmbB are required for the synthesis of arabinogalactan, and at least one enzyme (M. The scale of the problem is increasing, and the disease is becoming deadlier as it intersects with the spread of human immunodeficiency virus. The emergence of multidrug-resistant strains establishes the urgent need to fully understand the mechanisms of drug resistance. It is also effective in the treatment of opportunistic mycobacterial infections of patients with human immunodeficiency virus. The locus has been characterized; it consists of a regulator, EmbR, and two arabinosyltransferases, EmbA and EmbB (3). Most recently, work using isogenic strains has once again suggested that these mutations are linked to resistance (23). However, several lines of evidence suggest that EmbB is not the only target and that the target(s) may differ between mycobacterial species. Mycobacterium smegmatis was grown either in Lemco liquid medium (5 g liter−1 Lemco powder, 10 g liter−1 peptone, 5 g liter−1 NaCl) and 0. Kanamycin was used at 20 μg ml−1, hygromycin at 100 μg ml−1, and gentamicin at 10 μg ml−1 as required. For site-directed mutagenesis, amplification reactions were carried out in a 50-μl total volume containing 1× Pfu Ultra reaction buffer, 0. The thermocycling program used was 95°C for 1 min, followed by 18 cycles of 95°C for 1 min, 60°C for 1 min, and 68°C for 12 min, with a final extension cycle of 68°C for 20 min. A 5-μl volume of each reaction product was used to transform competent Escherichia coli. We previously demonstrated that high-efficiency replacement of L5-based integrating vectors occurs in M. We used this “switching” technique to test mutant alleles of embC for functionality in M. To confirm that vector replacement rather than cointegration had occurred, 24 transformants from each transformation were patch tested for gentamicin resistance, and all were gentamicin sensitive, confirming that the original plasmid was lost. Twenty microliters of exponential-phase liquid cultures was spotted onto agar in 12-well tissue culture plates. After 24 h of culture, cells were harvested, resuspended in 400 μl phenol-water (1:1), and incubated at 80°C for 2 h. One hundred microliters of chloroform was added, and 10 μl of the aqueous phase was analyzed in denaturing, nonreducing 16% acrylamide gels, followed by periodic acid-Schiff staining. After 14 days of culture, cells were harvested, resuspended in 400 μl phenol-water (1/1), and incubated at 80°C for 2 h. Alignment of the glycosyltransferase motif regions of the three Emb proteins of M. Conserved amino acids are asterisked; residues of high and low similarity are indicated by colons and periods, respectively. The two aspartate codons (D293 and D294) and the methionine codon (M300) are boldfaced. To test if the allele retained functional arabinosyltransferase activity, we transformed this vector into the embC deletion strain of M. Recombinant strains carried single-copy integrated plasmids expressing EmbC alleles from the Ag85a promoter. We next determined whether the D294G allele could complement a chromosomal deletion in M. The plasmid carrying the D294G allele was introduced into the del-int strain using a gene-switching method (19) so that the wild-type allele was replaced with the mutated allele, i. Replacement of the integrated wild-type gene with the D294G allele was achieved with high efficiency, indicating that this was indeed a functional allele that could support growth. Thus, we confirmed that the D294G mutation reduces, but does not completely abolish, the arabinosyltransferase activity of EmbC and that the glycosyltransferase motif identified by sequence homology is functional. The three arabinosyltransferases have conserved regions, including the region around codon 306 (Fig. All of the alleles were functional, in that they supported bacterial growth (Table 1). Sensitivity to other antibiotics (ampicillin, isoniazid, rifampin) remained unchanged (results not shown), excluding the possibility that this is a general permeability effect. The recovered plasmids all had different deletions, with at least 1 kb of the embC gene missing at either the 5′ or the 3′ end; in addition, most deletions resulted in a downstream frameshift. Again, the transformation efficiencies were low, and recovered plasmids had deletions in the embC gene. Transformation with the wild-type allele resulted in a low frequency of transformants (none of which expressed the protein, as determined by Western blotting [data not shown]). The wild-type strain had a reproducible cutoff point of 3 μg/ml in this assay using different inocula. Recombinant strains carried multicopy plasmids expressing embC alleles from the strong constitutive hsp60 promoter. Thus, although resistance was seen, its level was not as high as that of the resistance engendered by overexpression of embC. This has implications for the detection of clinical resistance and suggests that studies to look at the role of embC mutations in mediating clinically relevant phenotypes should be extended. Since inocula are adjusted and viable bacilli counted, the proportion method corrects for small deviations in the inoculum size and growth rate that could be masked in growth as spots or lawns. We used a rapid method for determining whether EmbC mutations resulted in changes in resistance, relying on spotting log-phase cultures onto drug plates and scoring for growth as a lawn. A comparison of the two methods using a subset of strains (Table 1) confirmed that the trends in the results were the same, i. EmbC is an integral membrane protein with a large number of transmembrane domains, making it extremely challenging to purify the active enzyme from whole cells. EmbB mutations are often associated with high-level resistance in clinical isolates, but mutations in codon 306 are not sufficient on their own to generate high-level resistance (23), so presumably there are secondary mutations (which may be dependent on strains already having EmbB mutations). In support of this, a recent study showed that a combination of mutations in EmbB codon 306 and EmbC codon 270 resulted in higher levels of resistance (11). In the future, it would be interesting to determine whether particular combinations of EmbB and EmbC mutations can give rise to high-level resistance. In this scenario, overexpression of either target could lead to resistance, simply by virtue of by binding excess drug. Thus, low-level resistance could be mediated by a mutation in either target protein via a titration effect, i. However, we think this is unlikely, since resistance to the other antibiotics tested remained the same. For antibiotics that target components of the cell wall, it is hard to distinguish between direct and indirect effects on resistance levels. Most notably, any one of the three genes can be deleted in the latter, while it is highly likely that all three are independently essential in the former. Roles of conserved proline and glycosyltransferase motifs of EmbC in biosynthesis of lipoarabinomannan. Recognition of multiple effects of ethambutol on metabolism of mycobacterial cell envelope. The role of the embA and embB gene products in the biosynthesis of the terminal hexaarabinofuranosyl motif of Mycobacterium smegmatis arabinogalactan.
As Nitrofurantoin belongs to virus ebola en francais nitrofurantoin 50 mg fast delivery the group of Antibacterials xnl antibiotic generic nitrofurantoin 50 mg online, it will have the following interactions: • Typhoid Vaccine (oral): Antibacterials inactivate oral typhoid vaccine antibiotic resistance threats cdc 50mg nitrofurantoin otc. Nitrofurantoin may cause dizziness and drowsiness and the patient should not drive or operate machinery if affected this way bacteria that causes diarrhea buy nitrofurantoin 50mg without prescription. A tabulated list of undesirable effects is outlined below: The undesirable effects are listed according to organ systems and following frequencies: Rare (≥1/10,000 to Not known (cannot be estimated from the available data) System organ class Frequency Adverse reaction Infections and infestations Not known Superinfections by fungi or resistant organisms such as Pseudomonas. However, these are limited to the genitourinary tract Blood and lymphatic system disorders Rare Not known Aplastic anaemia Agranulocytosis, leucopenia, granulocytopenia, haemolytic anaemia, thrombocytopenia,glucose¬6-phosphatedehydrogenase deficiency anaemia, megaloblastic anaemia and eosinophilia Immune system disorders Not known Allergic skin reactions, angioneurotic oedema and anaphylaxis Psychiatric disorders Not known depression, euphoria, confusion, psychotic reactions Nervous system disorders Not known Peripheral neuropathy including optic neuritis (sensory as well as motor involvement), nystagmus, vertigo, dizziness, headache and drowsiness. Benign intracranial hypertension Cardiac Rare Collapse and cyanosis Respiratory, thoracic and mediastinal disorders Not known Acute pulmonary reactions, Subacute pulmonary reactions* Chronic pulmonary reactions Cough, Dyspnoea, Pulmonary fibrosis; possible association with lupus-erythematous-like syndrome. Gastrointestinal disorders Not known Sialadenitis, Pancreatitis, Nausea, Anorexia, Emesis, Abdominal pain and Diarrhea. Chronic pulmonary reactions occur rarely in patients who have received continuous therapy for six months or longer and are more common in elderly patients. Monitoring of full blood count, liver function, and pulmonary function tests are recommended. The controlled crystal size is designed to control the speed of absorption and thus reduce the incidence of nausea. This special formulation of Nitrofurantoin had not caused any decrease in antibacterial efficacy. The capsule shell contains quinoline yellow (E104), titanium dioxide (E171), gelatin, sodium lauryl sulphate. How it works Nitrofurantoin is an antibacterial agent with a large crystal structure (called a macrocrystal) which restricts absorption through the gastrointestinal tract allowing nitrofurantoin to concentrate in urine. Nitrofurantoin belongs to the class of medicines known as nitrofuran antibacterials. Upsides May be used as a treatment for urinary tract infections or at a lower dosage to reduce the recurrence of urinary tract infections. Nitrofurantoin is effective for treating certain gram-negative and gram-positive urinary tract infections, such as those due to Escherichia coli, Enterococci, Staphylococcus aureus and susceptible strains of Klebsiella and Enterobacter. Because nitrofurantoin concentrates in urine, side effects are generally less than with other agents typically used to treat urinary tract infections. Unlike many other antibiotics, resistance to nitrofurantoin has never been a significant problem; experts believe its broad spectrum of action offers a protective effect against resistance development. However, some bacteria are not susceptible to nitrofurantoin and care should still be taken not to encourage the development of resistant bacteria. Downsides If you are between the ages of 18 and 60, take no other medication or have no other medical conditions, side effects you are more likely to experience include: Nausea or vomiting, changes in facial skin color, dark colored urine, flatulence, headache and weight loss. Other side effects, such as abdominal pain, constipation, diarrhea, skin reactions, or cardiovascular effects are uncommon or relatively rare. Nitrofurantoin has been associated with potentially fatal lung conditions such as interstitial pneumonitis and pulmonary fibrosis. The risk is greater in people receiving nitrofurantoin for longer than six months. Not suitable for people with significantly impaired kidney function or in those with a previous history of liver problems associated with nitrofurantoin use. Should not be used in pregnant patients near term (38 to 42 weeks gestation) or when labor is imminent, or in newborns aged less than one month, because of the risk of hemolytic anemia. Because the distribution of nitrofurantoin to other tissues is limited, there is a higher chance that the bacterial infection being treated may persist or recur. Should not be taken again by people who have had liver problems or reactions to nitrofurantoin in the past. Long-term use has also been associated with peripheral neuropathy (nerve disease or damage particularly confined to the feet or hands). The risk is greater in people with kidney disease, anemia, diabetes, electrolyte imbalance, vitamin B deficiency or with chronic debilitating diseases. May also cause other serious side effects such as hemolytic anemia (risk is greater in people with glucose-6-phosphate deficiency) and Clostridium difficile infection (symptoms include persistent diarrhea). May interact with quinolone antibiotics, and antacids that contain magnesium may reduce the absorption of nitrofurantoin. Probenecid and sulfinpyrazone can inhibit the excretion of nitrofurantoin, which may increase the risk of toxicity and decrease its effectiveness because this lowers the concentration of nitrofurantoin in the urinary tract. Bottom Line Nitrofurantoin is an effective antibiotic with a low risk of inducing bacterial resistance that is used specifically to treat urinary tract infections caused by susceptible bacteria. Tips Take with food to enhance absorption and decrease the risk of side effects such as nausea. Ensure you finish the course as prescribed to decrease the risk of resistant bacteria developing. Do not take antacid or indigestion remedies containing magnesium trisilicate at the same time as taking nitrofurantoin. Nitrofurantoin should only be used to treat infections caused by susceptible bacteria; it does not treat infections caused by viruses. Talk with your doctor if you develop watery or bloody stools with or without other symptoms such as stomach cramps or fever either while taking nitrofurantoin or within two months of discontinuing it. Do not take nitrofurantoin if you are in the last two to four weeks of your pregnancy. Measure the exact dose and then swallow (may be mixed with water, milk or fruit juice before swallowing). Tell any health professional that treats you that you are taking nitrofurantoin as it may interfere with laboratory tests. Response and Effectiveness The macrocrystalline form of nitrofurantoin allows nitrofurantoin to be absorbed more slowly, reducing any negative effects on the stomach (and decreasing the risk of nausea). An improvement in symptoms may be noticed within a couple of days; however, it is important the course of nitrofurantoin is finished or the drug continues to be taken for at least three days following a clear urine sample. Interactions Medicines that interact with nitrofurantoin may either decrease its effect, affect how long it works for, increase side effects, or have less of an effect when taken with nitrofurantoin. An interaction between two medications does not always mean that you must stop taking one of the medications; however, sometimes it does. Note that this list is not all-inclusive and includes only common medications that may interact with nitrofurantoin. You should refer to the prescribing information for nitrofurantoin for a complete list of interactions. Further information Remember, keep this and all other medicines out of the reach of children, never share your medicines with others, and use nitrofurantoin only for the indication prescribed. Medical Disclaimer Nitrofurantoin belongs to the class of medications called antibiotics. It is used to treat urinary tract infections or bladder infections caused by certain types of bacteria. The recommended dose of this medication for adults and children over 12 years old is 50 mg to 100 mg 4 times daily. Nitrofurantoin should be taken with food or milk to reduce the risk of stomach upset. It is calculated as 5 mg to 7 mg per kilogram of body weight per day, divided into 4 equal doses. Do not take nitrofurantoin if you: are allergic to nitrofurantoin or any ingredients of the medication have significantly reduced kidney function are a pregnant woman in labour or a pregnant woman expecting to go into labour soon (i. Check with your doctor as soon as possible if any of the following side effects occur: confusion hair loss mood swings, unusual thoughts, or unusual behavior rapid, uncontrolled movement of the eyes symptoms of liver problems (such as yellow eyes or skin, abdominal pain, pale stools, dark urine, itching, nausea, or fatigue) symptoms of low white blood cells (such as fever and chills or frequent infections) symptoms of low red blood cells (such as fatigue, weakness, decreased energy, or pale skin) symptoms of a lung reaction to the medication (such as fever, chills, cough, chest pain, or difficulty breathing) symptoms of nerve damage (such as tingling, burning, pain, or numbness in the arms and legs; or difficulty controlling the muscles in the arms or legs) Stop taking the medication and seek immediate medical attention if any of the following occur: symptoms of a serious skin reaction (such as a severe blistering skin rash that causes the skin to peel or fall off; fever; or bloodshot eyes) symptoms of a severe allergic reaction (such as hives, difficulty breathing, and swelling of the face or throat) Some people may experience side effects other than those listed. Bacterial resistance: Misuse of an antibiotic such as nitrofurantoin may lead to the growth of resistant bacteria that will not be killed by the antibiotic. Although you may begin to feel better early in your course of treatment with nitrofurantoin, you need to take the full course exactly as directed to finish ridding your body of the infection and to prevent resistant bacteria from taking hold. Do not take nitrofurantoin or other antibiotics to treat a viral infection such as the common cold; antibiotics do not kill viruses, and using them to treat viral infections can lead to the growth of resistant bacteria. Discolouration of urine: This medication may turn your urine a rust yellow or brown colour.
Azithromycin may be preferred if the use of a macrolide antibiotic is necessary in a patient receiving felodipine therapy medicine for dog uti over the counter buy nitrofurantoin us. Fentanyl: (Moderate) Consider a reduced dose of fentanyl with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary virus yole nitrofurantoin 50 mg mastercard. If erythromycin is discontinued antimicrobial insulation discount 50 mg nitrofurantoin overnight delivery, consider increasing the fentanyl dose until stable drug effects are achieved and monitor for evidence of opioid withdrawal antibiotics for acne bactrim buy nitrofurantoin line. If erythromycin is discontinued, fentanyl plasma concentrations will decrease resulting in reduced efficacy of the opioid and potential withdrawal syndrome in a patient who has developed physical dependence to fentanyl. Fluconazole: (Major) Caution is warranted with the coadministration of fluconazole and erythromycin. A small study of 13 healthy subjects resulted in a 40% increase in salmeterol maximum concentrations (Cmax) during concurrent repeat-dose administration of erythromycin. The effects of salmeterol on the cardiovascular system, as well as side effects like headache, tremor, and nervousness, may be potentiated. However, according to the manufacturer, coadministration of erythromycin did not significantly alter the pharmacokinetic disposition of fluvastatin. Food: (Moderate) The incidence of marijuana associated adverse effects may change following coadministration with erythromycin. Fosamprenavir: (Moderate) Caution is warranted with the concomitant use of erythromycin and fosamprenavir as increased fosamprenavir serum concentrations may occur. Cases ofTdP have been spontaneously reported during postmarketing surveillance in patients receiving erythromycin. Glecaprevir; Pibrentasvir: (Moderate) Caution is advised with the coadministration of glecaprevir and erythromycin as coadministration may increase serum concentrations of both drugs and increase the risk of adverse effects. Glecaprevir and erythromycin are both substrates and inhibitors of P-glycoprotein (P-gp). Both pibrentasvir and erythromycin are substrates and inhibitors of P-glycoprotein (P-gp). Goserelin: (Major) Consider whether the benefits of androgen deprivation therapy (i. In patients who complain of caffeine related side effects, the dosage of caffeine containing products may need to be reduced. Guaifenesin; Hydrocodone: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. Guaifenesin; Hydrocodone; Pseudoephedrine: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. Guanfacine: (Major) Erythromycin may significantly increase guanfacine plasma concentrations. Halogenated Anesthetics: (Major) Halogenated anesthetics should be used cautiously and with close monitoring with erythromycin. It is prudent to use caution and carefully weighing the risks and benefits of these agents versus alternative treatment options. Histrelin: (Major) Consider whether the benefits of androgen deprivation therapy (i. Homatropine; Hydrocodone: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. If erythromycin is discontinued, hydrocodone plasma concentrations will decrease resulting in reduced efficacy of the opioid and potential withdrawal syndrome in a patient who has developed physical dependence to hydrocodone. Hydrocodone: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. Hydrocodone; Ibuprofen: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. Hydrocodone; Phenylephrine: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. Hydrocodone; Potassium Guaiacolsulfonate: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. Hydrocodone; Potassium Guaiacolsulfonate; Pseudoephedrine: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. Hydrocodone; Pseudoephedrine: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. Therefore, the dose of corticosteroid should be titrated to avoid steroid toxicity. Ibuprofen; Oxycodone: (Moderate) Consider a reduced dose of oxycodone with frequent monitoring for respiratory depression and sedation if concurrent use of erythromycin is necessary. Ifosfamide: (Moderate) Monitor for a decrease in the efficacy of ifosfamide if coadministration with erythromycin is necessary. Imatinib: (Moderate) Any agent that inhibits cytochrome P450 3A4, such as erythromycin, may decrease the metabolism of imatinib and increase imatinib concentrations leading to an increased incidence of adverse reactions. Coadministration of indacaterol inhalation powder 300 mcg (single dose) with erythromycin (400 mcg qid x 7 days) resulted in a 1. The effects of indacaterol on the cardiovascular system, and side effects like headache, tremor, or nervousness may be potentiated. Isavuconazonium: (Moderate) Caution is warranted as concomitant use of isavuconazonium and erythromycin may result in increased isavuconazonium serum concentrations. Coadministration of oral erythromycin 500 mg and rifampin 600 mg to healthy patients led to a reduced erythromycin maximum serum concentration (Cmax) and an increased clearance. Isradipine: (Major) Avoid administration of erythromycin and isradipine, particularly in geriatric patients. Azithromycin may be preferred if the use of a macrolide antibiotic is necessary in a patient receiving isradipine therapy. Coadministration may result in increased plasma concentrations of itraconazole, thereby further increasing the risk for adverse events. Ivabradine: (Major) Avoid coadministration of ivabradine and erythromycin as increased concentrations of ivabradine are possible. Ivacaftor: (Major) If erythromcyin and ivacaftor are taken together, administer ivacaftor at the usual recommended dose but reduce the frequency to once daily. Caution is recommended if ixabepilone is coadministered with erythromycin; closely monitor patients for ixabepilone-related toxicities. Coadministration may result in increased plasma concentrations of ketoconazole, thereby further increasing the risk for adverse events. Ledipasvir; Sofosbuvir: (Moderate) Caution and close monitoring of adverse reactions is advised with concomitant administration of erythromycin and ledipasvir; sofosbuvir. Both ledipasvir and erythromycin are substrates and inhibitors of the drug transporter P-glycoprotein (P-gp); sofosbuvir is a P-gp substrate. Taking these drugs together may increase plasma concentrations of all three drugs. According to the manufacturer, no dosage adjustments are required when ledipasvir; sofosbuvir is administered concurrently with P-gp inhibitors. Lemborexant: (Major) Avoid coadministration of lemborexant and erythromycin as concurrent use is expected to significantly increase lemborexant exposure and the risk of adverse effects. Letermovir: (Moderate) Caution is warranted with the concurrent administration of erythromycin and letermovir, as this may result in increased concentrations of letermovir. Leuprolide: (Major) Consider whether the benefits of androgen deprivation therapy (i. Leuprolide; Norethindrone: (Major) Consider whether the benefits of androgen deprivation therapy (i. Levamlodipine: (Major) Avoid administration of erythromycin and amlodipine, particularly in geriatric patients. Additionally, rare cases of TdP have been spontaneously reported during postmarketing surveillance in patients receiving levofloxacin. Lithium: (Major) Lithium should be used cautiously and with close monitoring with erythromycin. Lomitapide: (Severe) Concomitant use of erythromycin and lomitapide is contraindicated. If treatment with erythromycin is unavoidable, lomitapide should be stopped during the course of treatment.
In a drug interaction study antimicrobial ingredients cheap nitrofurantoin online visa, ketoconazole decreased the active metabolite of clopidogrel antimicrobial waiting room chairs discount nitrofurantoin online. Cobicistat: (Major) Avoid concurrent use of ketoconazole with regimens containing cobicistat and atazanavir or darunavir antimicrobial therapy inc purchase genuine nitrofurantoin on line. Cobimetinib: (Major) Avoid the concurrent use of cobimetinib with ketoconazole due to antibiotic creams buy 50mg nitrofurantoin otc the risk of cobimetinib toxicity. Discontinuation of ketoconazole could decrease codeine plasma concentrations, decrease opioid efficacy, and potentially lead to a withdrawal syndrome in those with physical dependence to codeine. Colchicine: (Major) Due to the risk for serious colchicine toxicity including multi-organ failure and death, avoid coadministration of colchicine and ketoconazole in patients with normal renal and hepatic function unless the use of both agents is imperative. Specific dosage adjustment recommendations are available for the Colcrys product for patients who have taken ketoconazole in the past 14 days or require concurrent use: for prophylaxis of gout flares, if the original dose is 0. Colchicine; Probenecid: (Major) Due to the risk for serious colchicine toxicity including multi-organ failure and death, avoid coadministration of colchicine and ketoconazole in patients with normal renal and hepatic function unless the use of both agents is imperative. Coadministration is contraindicated in patients with renal or hepatic impairment because colchicine accumulation may be greater in these populations. Conivaptan: (Severe) Coadministration of conivaptan with ketoconazole is contraindicated. The effect of coadministration of ketoconazole with intravenous conivaptan has not been studied. Copanlisib: (Major) Avoid the concomitant use of copanlisib and ketoconazole if possible; increased copanlisib exposure may occur. If coadministration cannot be avoided, reduce the copanlisib dose to 45 mg and monitor patients for copanlisib-related adverse events (e. If concomitant use is unavoidable, reduce the dose of crizotinib to 250 mg by mouth once daily. Cyclosporine: (Major) The interactions between cyclosporine and systemic azole antifungals (e. Cyclosporine concentrations may increase within 1 to 3 days after starting azole antifungal therapy, and may persist for > 1 week after discontinuing antifungal treatment. Ketoconazole can increase cyclosporine concentrations up to 3-fold within days of addition of ketoconazole to cyclosporine therapy. It takes about 7 to 10 days for cyclosporine concentrations to normalize after stopping ketoconazole. Ketoconazole has been documented to lower the daily maintenance dosage of cyclosporine, thus reducing the overall cost of therapy; however, this approach is not routinely used. Close monitoring of cyclosporine concentrations is required when given in combination with systemic azole antifungals; a 50% reduction in cyclosporine dosage may be required. Dabigatran: (Major) Increased serum concentrations of dabigatran are possible when dabigatran, a P-glycoprotein (P-gp) substrate, is coadministered with ketoconazole, a P-gp inhibitor. When used in patients with non-valvular atrial fibrillation, avoid the coadministration of dabigatran and systemic ketoconazole in patients with severe renal impairment (CrCl less than 30 mL/minute), and consider reducing the dabigatran dose to 75 mg twice daily when ketoconazole and dabigatran are coadministered in patients with moderate renal impairment (CrCl 30 to 50 ml/min). Coadministration of dabigatran and ketoconazole results in increased dabigatran serum concentrations and, therefore, an increased risk of bleeding. P-gp inhibition and renal impairment are the major independent factors that result in increased exposure to dabigatran. Dabrafenib: (Major) Avoid the concomitant use of dabrafenib and ketoconazole; dabrafenib exposure increased by 71% when these drugs were administered together in a drug interaction study. Additionally, the concentrations of ketoconazole may be decreased resulting in loss of efficacy. If concomitant use cannot be avoided, monitor patients for dabrafenib toxicity (e. Taking these drugs together may increase daclatasvir serum concentrations, and potentially increase the risk for adverse effects. Darolutamide: (Moderate) Monitor patients more frequently for darolutamide-related adverse reactions if coadministration with ketoconazole is necessary due to the risk of increased darolutamide exposure; decrease the dose of darolutamide for grade 3 or 4 adverse reactions or for otherwise intolerable adverse reactions. Darunavir; Cobicistat: (Major) Avoid concurrent use of ketoconazole with regimens containing cobicistat and atazanavir or darunavir. Concomitant systemic use of ketoconazole with darunavir may increase plasma concentrations of darunavir. Darunavir; Cobicistat; Emtricitabine; Tenofovir alafenamide: (Major) Avoid concurrent use of ketoconazole with regimens containing cobicistat and atazanavir or darunavir. Dasabuvir; Ombitasvir; Paritaprevir; Ritonavir: (Major) When administering ketoconazole with ritonavir or ritonavir-containing drugs, do not exceed the maximum recommended ketoconazole dose of 200 mg per day. An alternative to ketoconazole with no or minimal enzyme inhibition potential is recommended if possible. If dasatinib is not tolerated after dose reduction, either discontinue ketoconazole or stop dasatinib until ketoconazole is discontinued. Allow a washout of approximately 1 week after ketoconazole is stopped before increasing the dasatinib dose or reinitiating dasatinib. Deflazacort: (Major) Decrease deflazacort dose to one third of the recommended dosage when coadministered with ketoconazole. Trough plasma concentrations of delavirdine may be increased by about 50% in patients receiving ketoconazole concurrently with delavirdine. Dexamethasone: (Moderate) Coadministration may result in increased exposure to dexamethasone and increased corticosteroid-related adverse effects. Ketoconazole has been reported to decrease the metabolism of certain corticosteroids by up to 60%. In addition, ketoconazole alone can inhibit adrenal corticosteroid synthesis and may cause adrenal insufficiency during corticosteroid withdrawal. Coadministration results in increased quinidine serum concentrations, with potential to result in proarrhythmias. A single case report has documented substantial elevations in serum quinidine concentrations after the addition of ketoconazole. Until more data are available, ketoconazole should be considered contraindicated in patients receiving quinidine. Dichlorphenamide: (Moderate) Use dichlorphenamide and ketoconazole together with caution. Dichlorphenamide increases potassium excretion and can cause hypokalemia and should be used cautiously with other drugs that may cause hypokalemia including antifungals. If hypokalemia occurs or persists, consider reducing the dichlorphenamide dose or discontinuing dichlorphenamide therapy. Didanosine, ddI: (Major) Administer ketoconazole at least 2 hours before or several hours after didanosine chewable tablets and powder for oral solution. Didanosine chewable tablets and powder for oral solution contain acid buffers to enhance the bioavailability of didanosine. These buffers, however, may decrease the absorption of ketoconazole, which requires an acid environment for absorption. The delayed-release didanosine capsules do not contain a buffering agent and would not be expected to interact with ketoconazole. Digoxin: (Moderate) Concomitant use of digoxin with ketoconazole has resulted in increased digoxin serum concentrations. Plasma concentrations of digoxin should be monitored closely if ketoconazole is added. Exercise caution when co-administering systemic azole antifungals and calcium-channel blockers. Diphenhydramine; Hydrocodone; Phenylephrine: (Moderate) Consider a reduced dose of hydrocodone with frequent monitoring for respiratory depression and sedation if concurrent use of ketoconazole is necessary. If ketoconazole is discontinued, hydrocodone plasma concentrations will decrease resulting in reduced efficacy of the opioid and potential withdrawal syndrome in a patient who has developed physical dependence to hydrocodone. Docetaxel: (Major) Avoid coadministration of docetaxel with ketoconazole if possible due to increased plasma concentrations of docetaxel. If concomitant use is unavoidable, closely monitor for docetaxel-related adverse reactions and consider a 50% dose reduction of docetaxel. Dofetilide: (Severe) Concurrent use of dofetilide with ketoconazole is contraindicated due to the risk of serious cardiovascular events. Conversely, ketoconazole concentrations are decreased when administered with rilpivirine. The plasma concentrations of donepezil may be elevated when administered concurrently with ketoconazole. Coadministration with ketoconazole increased mean donepezil concentrations by 36%. Doravirine: (Minor) Coadministration of doravirine and ketoconazole may result in increased doravirine plasma concentrations.
Buy cheap nitrofurantoin 50 mg on line. Norwex Product Training: EnviroCloth.